Out of all emergency department visits recorded, 80% involve corneal abrasion and foreign bodies. That’s a significant number of cases given that eye trauma accounts for three percent of all visits to the emergency department.
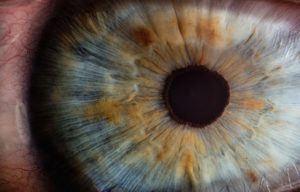 The cornea is the transparent layer that shields the front of the eye. It is the most likely casualty of eye injury due to its position in the eye.
The cornea is the transparent layer that shields the front of the eye. It is the most likely casualty of eye injury due to its position in the eye.
Maintaining a healthy lifestyle is imperative for healthy eyes. Exposing the eye to dirt and toxic pollutants can increase your risk of contracting a corneal disease. However, some conditions are genetically acquired.
Corneal disorders sometimes require transplantation. More than 33,000 Americans undergo the procedure every year to replace damaged corneas. However, many misunderstand corneal disease and the available treatments altogether.
A Healthy Cornea: How It Works
Unlike most of the other body tissues, the cornea does not have blood vessels. It relies on tears and the eye’s aqueous humor for nourishment and protection against infection.
The cornea has five membranes that protect the eye from foreign particles, germs, and dirt. They also filter out excessive radiation from the sun.
The cornea plays an essential role in vision. About 65% to 75% of the eye’s focusing power emanates from the cornea. It achieves this by controlling the light that enters the eye.
It refracts light onto the lens, which in turn refocuses the light onto the retina. The retina generates electrical impulses from the light.
Then, the optic nerve transmits the signals to the brain for interpretation. The brain then produces images.
Corneal Disease
A damaged cornea means impaired vision or blindness. Some of the most common corneal disorders are inherited conditions while others result from lifestyle issues. For instance, extended exposure to products that contain volatile organic compounds (VOC) can trigger corneal disease.
Most of the eye disorders that occur naturally come in the form of corneal dystrophies. Let’s have a look.
Corneal Dystrophies: What Are They?
Corneal dystrophies occur when a section or different parts of the cornea get clouded by a buildup of material. The disorders are usually inherited.
They don’t affect other parts of the body and have no relationship with other conditions ailing other organs. Corneal dystrophies affect both eyes and advance gradually.
People with corneal dystrophies can suffer from different scales of vision impairment. Some can experience severe vision problems while others only discover the disease during a routine checkup. Other patients undergo recurrent pain episodes, but the condition does not cause permanent blindness.
The most common types of corneal disease include Fuchs’ dystrophy, keratoconus, map-dot-fingerprint dystrophy, and lattice dystrophy.
- Fuchs’ Corneal Dystrophy
Fuchs’ dystrophy is a corneal disease that affects about four percent of people over 40 in the United States. Early signs and symptoms may start occurring in a person’s twenties but in rare circumstances.
The disease causes material known as guttae to accumulate in the middle of the cornea and spread all over. The deposits lead to the gradual death of the cells of the cornea resulting in the deterioration of vision.
Symptoms of Fuchs’ Dystrophy
Also known as Fuchs’ endothelial dystrophy, its very first sign is a blurred vision in the morning which disappears later in the day. Victims lose visual acuity (ability to see details) over time. They also cannot tolerate high-intensity light.
As the disease advances, zits can develop on the surface of the cornea. They become painful especially if they burst.
Other symptoms include a gritty-like feeling in the eyes, poor vision in humid weather, and swelling.
Fuchs’ dystrophy affects twice or more the number of women than men. Scientists have not discovered the reason for this trend.
Numbers of Fuchs’ dystrophy patients who require surgery at some point are hazy. Quantification becomes a challenge because various age groups have different trends in prevalence. Methods of diagnosis amongst doctors vary, and the treatment methods keep changing as well.
A study involving 16,535 patients showed that 992 people between 65 and 88 years needed a corneal transplant within six years. That represented six percent against five percent of patients in the 44 to 64 age bracket during the same period.
Treatment for Fuchs’ Dystrophy
Prescription eye drops or ointments help with the pain and swelling. If necessary, a doctor can also recommend contact lenses.
If the extent of corneal scarring warrants more intervention, a corneal transplant may be warranted.
- Keratoconus Dystrophy
This corneal disease deforms the cornea making it thinner than usual. It also bulges outwards to resemble cone shape.
The condition becomes worse over time. The patient can develop a blurred vision that no corrective lenses can improve, as well as myopia (nearsightedness). If not arrested, the affected person loses vision.
An eye exam can show iron deposits in the cornea appearing as a yellow-brownish ring (Fleischer ring) surrounding the iris. The affected eye may also develop thin white lines running vertically in the rear tissue of the cornea.
What Causes Keratoconus?
Keratoconus affects one in every 500 to 2000 people across the world. The primary cause of this corneal disease is not apparent. Scientists suspect genetic and environmental factors to be the triggers of this disease.
Some studies have linked the condition to inheritance. About seven percent of keratoconus patients have reported some history if the disease in their family
Repeated eye rubbing hastens the destruction of the cornea. Prolonged use of contact lenses on the thinned cornea also causes scarring. However, it is unclear if the rubbing and the use of contact lenses cause keratoconus or the habits aggravate an existent condition.
There is also a connection between allergic reactions and keratoconus. On average, more than 30% of people with this corneal disease suffer from allergies. Whether it’s the allergies that cause eye rubbing which in turn worsens keratoconus is unknown.
The disease can start in one eye before spreading the other. Either eye may exhibit different levels of severity. In most cases, signs and symptoms of keratoconus begin in adolescence and worsen towards mid-adulthood.
Correction Options for Keratoconus
In the early stages, keratoconus can be corrected with soft contact lenses or spectacles. An ophthalmologist can recommend special contact lenses to correct the cornea’s distortion if it worsens.
After this treatment, the cornea should stabilize in a few years. Some patients cannot tolerate the lenses, or the corneal scarring can become excessive. The most appropriate correction procedure for such cases is a corneal transplant.
- Map-Dot-Fingerprint Dystrophy
Also called the epithelial basement membrane dystrophy, this corneal disease causes the basement membrane to fold and develop abnormally. The basement membrane is the foundation on which the epithelial cells of the cornea anchor themselves.
When inspected using the slit lamp examination, the folds on the affected epithelium appear like maps and dots. Sometimes, the basement membrane forms concentric circles that look like fingerprint images.
The anomaly in the basement membrane prevents epithelial cells from attaching correctly. As a result, the cells get eroded, causing the outermost layer of the epithelium to rise a bit forming a small gap.
The disease is more prevalent in adults aged between 40 and 70 years, but it can affect a negligible percentage of younger persons.
The U.S. National Library of Medicine estimates that over 76% of individuals beyond 50 years are likely to have the map-dot-fingerprint dystrophy. The disease affects about 42% of people in all age groups. Similar statistics reflect in families with patients suffering from epithelial basement membrane dystrophy.
Some scientists have related this corneal disease to inheritance while others think that its prevalence depends on age.
Symptoms of Map-Dot-Fingerprint Dystrophy
Epithelial erosions can cause periodic blurring. The disorder also exposes nerve endings causing pain in the eyes that can last for several days. For most people, the pain is more severe in the morning hours than later in the day.
Other symptoms include the secretion of excessive tears, high sensitivity to light, and a feeling of foreign particles in the eyes. The symptoms usually occur and disappear on their own without causing permanent loss of vision. Some people can have this corneal disease but not experience any of the symptoms.
Treatment for Map-Dot-Fingerprint Dystrophy
If the condition requires treatment, eye doctors usually prescribe lubricating ointments and eye drops. Epithelial erosions heal in about three days, but the patient can experience sporadic flare-ups of the symptoms for several weeks.
Advanced corrective procedures for chronic cases include corneal scrapping on the eroded areas for fresh tissue to grow. Another method is phototherapeutic keratectomy which helps to clear surface irregularities. Finally, ophthalmologists can employ anterior corneal stromal punctures to improve the adherence of the epithelial cells to the basement membrane.
- Lattice Dystrophy
The cornea must remain clear for a person to see. In the case of lattice dystrophy, clumps of protein (amyloid deposits) accumulate in the stromal layer of the cornea leading to vision impairment. The deposits form a pattern of branching fibers which resemble a lattice.
Over time, the lattice lines overwhelm the stromal membrane. They become opaque and end up impairing the victim’s vision.
Recurrent corneal erosions can develop in the eyes due to the separation of the various membranes of the cornea.
This corneal disease comes as a result of genetic mutations. Some descendants of families with a history of lattice dystrophy are likely to develop the disorder.
One copy of an altered gene in a cell is enough to cause the condition. In most cases, an affected person has at least one parent with lattice dystrophy.
Around six percent of the population can contract lattice degeneration. It’s a risk factor for retinal tearing and detachment although most patients do not get these problems.
Symptoms of Lattice Dystrophy
Individuals with lattice dystrophy, in most cases, experience corneal erosions which cause severe pain. The eyes can also become photophobic (sensitive to bright light).
Lattice dystrophy is a bilateral corneal disease, meaning it affects both eyes. The disorder usually begins in childhood when a person is between two and seven years. It progresses to cause vision problems later in adulthood.
Treatment for Lattice Dystrophy
For patients undergoing pain, the doctor can recommend eye drops or ointments to patients. The medicine lubricates the cornea to reduce its friction against the eyelid. An eye patch may also be necessary to restrain the movement of the eyelid.
Corneal erosions heal in under a week if no complications occur. However, the patient can have some discomfort or pain for about seven weeks.
Some patients with lattice dystrophy develop so much scarring under the epithelium by the age forty that it affects vision significantly. At this point, corneal transplantation may be the ideal treatment. Lattice dystrophy can still reappear later in life even after successful corneal transplantation.
Corneal Transplantation and Its Success
Cornea transplantation is a surgical procedure that replaces part of the cornea with donor tissue. It helps to reverse or control the effects of the corneal disease. It can restore vision, relieve pain, and reinstate the appearance of a damaged cornea.
According to studies, the success rate of corneal transplantation in favorable subjects may be higher than 90%. The treated eye acquires good visual acuity after the operation.
The rate can drop to between 10 and 20 percent in unfavorable subjects. The leading cause of graft failure is rejection, which accounts for 34%. Infection and glaucoma account for 34% and 18% respectively.
Wrap Up
The list of corneal disease is extensive. It features unpreventable degeneration as well as infections caused by germs. Some are curable while others are not.
Different corneal disorders exhibit themselves in unique ways, but some symptoms replicate. Some of the typical signs of eye disease are pain, blurred vision, extreme sensitivity, redness, and gritty feeling.
Hygiene is essential for healthy eyes. Improper cleaning or use of contact lenses, for example, can aggravate your condition or cause secondary infections.
For hereditary conditions, early detection can help save your vision. A skilled ophthalmologist can correct the disorders.
Contact experienced eye doctors for an examination for more information and avoid the risk of vision loss.